Healthcare Professionals: Please login or sign-up for PRO Pricing HERE
TheraTogs Wunzi Infant System
$302.00 – $380.00
Product Details
Sizing
Standard Accessories
Technical Specs
Documents / Videos
FAQ
Product Details
The TheraTogs Wunzi Infant System, modeled after the well-known ‘onesie’ for babies, is tailored for infants weighing up to 26 lbs. It offers a personalized, comforting embrace that enhances trunk alignment and stabilizes the core.
Key Benefits:
- It takes a minute or less to dress your infant – even the wiggle-worms – in a Wunzi.
- The diaper flap goes on over the diaper, and lowers easily for lightning-quick diaper changes.
- Closure tabs are embedded right into the garment – so no loose tabs to keep track of.
- The two Wunzi components are machine-washable, air-dry.
- The “next-size-up” configuration allows you to make one purchase, keep up with the baby’s growth, and keep those TheraTogs benefits going.
Postural control is an essential component of early intervention
Babies build trunk and neck control/strength before they gain functional skills. Trunk control problems that occur in infancy typically lead to long-term developmental deficits in limb use and movement.
The Wunzi system is designed to help very young clients by increasing sensory input while improving core stability. One of our most popular products, it supports therapy goals both during and between therapy sessions, providing essential carry-over.
The base system includes limb cuffs and strapping to create optimal posture, and the add-on Limb Kit operates like external muscles and ligaments to improve functioning body and proximal joint alignment for better motor development.
Goes on in seconds & over diapers
Caregivers love the over-the-diaper design which is quick and easy to put on. Closure tabs are embedded right into the garment – no loose tabs to keep track of.
Like all TheraTogs systems, the Wunzi is a comfortable, foam-lined, Velcro®-sensitive garment and strapping system that grips the skin. The patented composite fabric is elasticized with a stretch bias that favours good postural alignment – excellent for a growing baby.
If you don’t see your indication in this list talk to your clinician or call us to see if the Wunzi might be right for you.
- Hypotonia
- Diplegic Cerebral Palsy
- Hemiplegic Cerebral Palsy
- Torticollis
- Athetosis
- Cerebellar Ataxia
- Obstetrical Brachial Plexus Injury (OBPI)
- Developmental Delay
Working together, the clinician and caregiver can achieve these and similar outcomes with the Wunzi Infant System:
- Increase sensory awareness and information
- Train functioning trunk muscles in shorter state to improve postural alignment and control
- Limit excessive trunk motions
- Improve functioning alignment of hips and/or shoulders
- Gently stabilize one or both scapulae
- Improve respiration by reducing flexible kyphosis
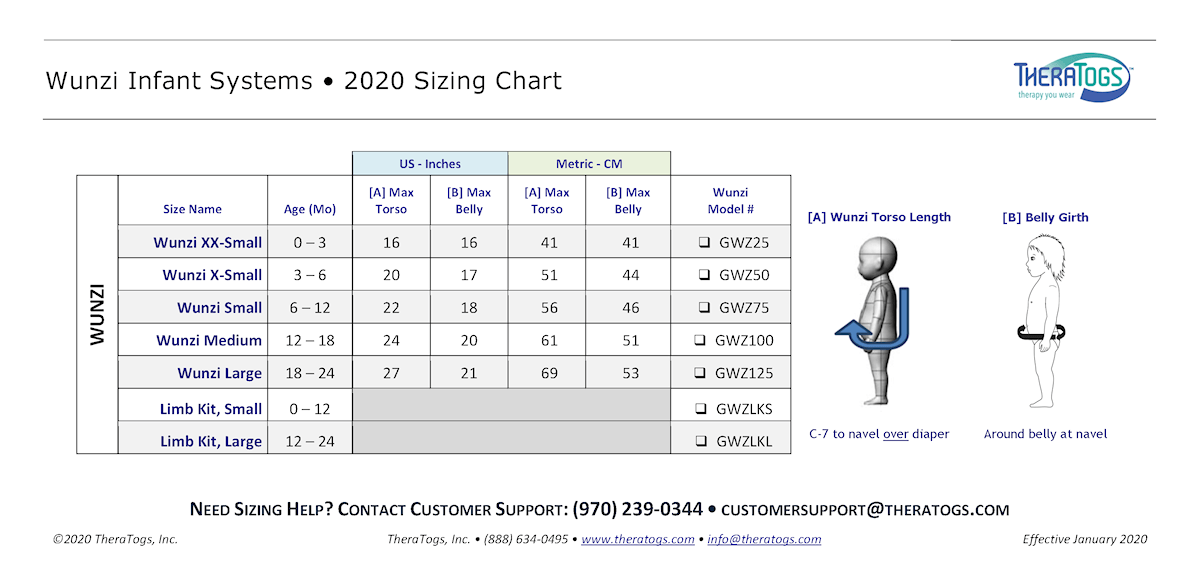
Sizing
For Torso Length measurement (expressed in inches), measure down from C-7 (the big bone at the bottom of the neck) over the diaper and up to the child’s navel as shown below. Be careful to wrap the tape gently over the diaper. For Belly Girth, measure the infant’s belly circumference at the navel (also in inches).
Standard Accessories
Technical Specs
Documents / Videos

Research
These references speak to the critical development of proper postural control and alignment in infants – which the TheraTogs Wunzi system is expressly designed to support:
Babik I, Galloway JC, Lobo MA. 2017. Infants born preterm demonstrate impaired exploration of their bodies and surfaces throughout the first 2 years of life. Phys Ther. 97(9):915-925.
Bly L. 2011. Components of Typical and Atypical Motor Development. Neurodevelopmental Treatment Association; www.ndta.org
Boxum AG, van Balen LC, Dijkstra LJ, et al. 2014. Postural adjustments in infants at very high risk for cerebral palsy before and after developing the ability to sit independently. Early Hum Dev. 90(9):435-41.
Brogren E, Hadders-Algra M, Forssberg H. 1998. Postural control in sitting children with cerebral palsy. Neurosci Biobehav Rev. 22(4):591-6. Review.
de Graaf-Peters VB, Blauw-Hospers CH, Dirks T, et al. 2007. Development of postural control in typically developing children and children with cerebral palsy: possibilities for intervention? Neurosci Biobehav Rev. 31(8):1191-2000. Review.
Dudek-Shriber L, Zelazny S. 2007. The effects of prone positioning on the quality and acquisition of developmental milestones in four-month-old infants. Pediatr Phys Ther. 19(1):48-55.
Dusing SC, Harbourne RT, Lobo MA, et al. 2019. a physical therapy intervention to advance cognitive and motor skills: a single subject study of a young child with cerebral palsy. Pediatr Phys Ther. 31(4):347-352.
Dusing SC, Izzo TA, Thacker LR, Galloway JC. 2014. Postural complexity differs between infant born full term and preterm during the development of early behaviors. Early Hum Dev. 90(3):149-56. Free PMC article.
Dusing SC, Thacker LR, Galloway JC. 2016. Infant born preterm have delayed development of adaptive postural control in the first 5 months of life. Infant Behav Dev. 44:49-58.
Feldman AG. 2016. The Relationship Between Postural and Movement Stability. Adv Exp Med Biol. 957:105-120. Review.
Gramsbergen A, Hadders-Algra M. 2005. Posture in the picture: on the relevance of postural control in children with developmental motor disorders. Summer, 2004. Groningen, The Netherlands. Neural Plast. 12(2-3):73-75. Free PMC article.
Green EM, Mulcahy CM, Pountney TE. 1995. An investigation into the development of early postural control. Dev Med Child Neurol. 37(5):437-48.
Hadders-Algra M, Brogren E, Forssberg H. 1998. Development of postural control–differences between ventral and dorsal muscles? Neurosci Biobehav Rev. 22(4):501-6. Review.
Hadders-Algra M, Carlberg EB. 2008. Postural Control: A Key Issue in Developmental Disorders (Clinics in Developmental Medicine), MacKieth Press (Wiley).
Hadders-Algra M. Neurosci Biobehav Rev. 2018. Early human motor development: From variation to the ability to vary and adapt. 90:411-427. Free article. Review.
Heathcock JC, Galloway JC. 2009. Exploring objects with feet advances movement in infants born preterm: a randomized controlled trial. Phys Ther. 89(10):1027-38. Free PMC article. Clinical Trial.
Hirabayashi S, Iwasaki Y. 1995. Developmental perspective of sensory organization on postural control. Brain Dev. 17(2):111-3.
Johnston MV. 2009. Plasticity in the developing brain: implications for rehabilitation. Dev Disabil Res Rev. 15(2):94-101.
Konishi Y, Takaya R, Kimura K, et al. 1994. Development of posture in prone and supine positions during the prenatal period in low risk preterm infants. Arch Dis Child Fetal Neonatal Ed. 70(3):F188-91. Free PMC article.
Lee HM, Galloway JC. 2012. Early intensive postural and movement training advances head control in very young infants. Phys Ther. 92(7):935-47. Clinical Trial.
Lobo MA, Kokkoni E, Cunha AB, Galloway JC. Infants born preterm demonstrate impaired object exploration behaviors throughout infancy and toddlerhood. Phys Ther. 2015;95(1):51-64.
Monterosso L, Kristjanson L, Cole J. 2002. Neuromotor development and the physiologic effects of positioning in very low birth weight infants. J Obstet Gynecol Neonatal Nurs. 31(2):138-46. Review.
Rocha NA, dos Santos Silva FP, de Toledo AM, Tudella E. 2009. Variability in the levels of postural control in 0-4-month-old infants. Infant Behav Dev. 32(4):376-80.
Rocha NA, Tudella E. 2008. The influence of lying positions and postural control on hand-mouth and hand-hand behaviors in 0-4-month-old infants. Infant Behav Dev. 31(1):107-14.
Steindl R, Kunz K, Schrott-Fischer A, Scholtz AW. 2006. Effect of age and sex on maturation of sensory systems and balance control. Dev Med Child Neurol. 48(6):477-82.
Sweeney JK, Gutierrez T. 2002. Musculoskeletal implications of preterm infant positioning in the NICU. J Perinat Neonatal Nurs. 16(1):58-70.Review.
Vaivre-Douret L, Ennouri K, Jrad I, Garrec C, Papiernik E. 2004. Effect of positioning on the incidence of abnormalities of muscle tone in low-risk, preterm infants. Eur J Paediatr Neurol. 8(1):21-34. Clinical Trial.
van Balen LC, Dijkstra LJ, Dirks T, Bos AF, Hadders-Algra M. 2019. Early Intervention and Postural Adjustments During Reaching in Infants at Risk of Cerebral Palsy. Pediatr Phys Ther. 31(2):175-183.
van Balen LC, Boxum AG, Dijkstra LJ, et al. 2018. Are postural adjustments during reaching related to walking development in typically developing infants and infants at risk of cerebral palsy? Infant Behav Dev. 50:107-115.
FAQ
What is a TheraTogs “Wunzi” System?
The Wunzi is an innovative TheraTogs system for infants, crafted to assist children from their first days up to 24 months who require support for posture, sensorimotor stimulation, or neuromotor rehabilitation. It’s crafted for easy application on a child, and its user-friendly design makes it a breeze for caregivers. Mimicking the popular “onesie” style commonly worn by infants, the Wunzi is aptly named and uniquely tailored for the little ones. Notably, it stands as the sole neuromotor rehabilitation system exclusively developed for infants. Additionally, all components of the Wunzi are free from latex.
How can I determine if the Wunzi is an appropriate choice for my child or for a child under my care?
From birth to age three is a crucial period for addressing any signs of developmental delays. A trained therapist or a vigilant caregiver can spot these delays by comparing them to typical early baby milestones. It’s important to note that neuromotor development is closely linked to sensorimotor development. A Wunzi is suitable for children or clients under 24 months who show signs of motor or sensory developmental delays. These signs may include difficulty in maintaining symmetrical body or head positions, challenges in holding steady head, trunk, or hip positions, an inability to regain balance during usual movements, low muscle tone or “floppiness” in the trunk, and a positive response to being hugged and held in age-appropriate postures.
In what sizes is Wunzi available?
The Wunzi comes in five different sizes, catering to children who weigh approximately 7 to 26 pounds (around 3 to 12 kilograms). It is suitable for newborns and can be used up until roughly 24 months of age.
What specific clinical conditions or symptoms indicate that using a Wunzi would be beneficial?
The Theratogs Wunzi can be effectively used for a variety of clinical conditions and symptoms. These include Hypotonia, which is characterized by reduced muscle tone, and Cerebellar Ataxia, a condition that impacts coordination. It’s also suitable for children with Diplegic and Hemiplegic Cerebral Palsy, both of which affect muscle control and coordination. Children with Athetosis, known for causing involuntary movements, can benefit from it as well. Additionally, it’s helpful for infants experiencing Torticollis, a condition leading to a tilted or twisted neck, and those who have suffered a Brachial Plexus Injury, impacting arm and hand movement. Lastly, the Wunzi is beneficial for children showing signs of Developmental Delay, assisting in their growth and motor skill development.
Does the Wunzi come with guidelines for dressing and usage?
The fundamental Wunzi system is straightforward to use. However, basic instructions are included in the package, and there is also an instructional video available under the Video tab.
How do I measure my child or client for a TheraTogWunzi?
Please refer to the sizing table on the Remington Medical Wunzi page.
Can the Wunzi be worn over a diaper, and is it designed for everyday use?
The Wunzi is intentionally crafted to fit over a diaper—indeed, it’s advised not to use the Wunzi without a diaper! Its soft foam surface is kind to an infant’s skin, and the special stretch fabric composite is designed for comfort, allowing it to be worn for as many hours a day as necessary.
Is it possible to use a Wunzi for my child or client who has a G-tube?
Absolutely, you can. The Wunzi is crafted from our patented and unique GoldTone™ material, which allows for trimming or perforation without any fraying or loss of functionality. Additionally, the garment’s Velcro-sensitive surface can be utilized to securely position the G-tube.
How should I wash and maintain my Wunzi?
The Wunzi system is designed to be machine washable on a gentle cycle and should be washed at least once a week without any detergent. Extra care should be taken when handling the garments while they’re wet, as the foam’s soft and gentle properties also make it susceptible to nicks or chips when damp. Comprehensive care and washing instructions in English are provided with your system. Additionally, care instructions in Spanish can be found under the documents tab on this product page. For any specific product care inquiries, you should reach out to our support team.













